With commentary by

Paul Forsberg, PharmD, MHA, BCOP
Director of Pharmacy and
Compliance Officer
Minnesota Oncology
St. Paul, MN

Sanjiv Agarwala, MD
Chief of Medical Oncology and Hematology
Temple University School of
Medicine, Philadelphia, PA
Introduction
Melanoma is the fifth leading cancer diagnosis, corresponding to 5.2% of all new cancer diagnoses and the cause of most skin cancer deaths.1,2 In 2022, there will be an estimated 99,780 new melanoma cases and 7650 deaths.2,3 Groups most affected include non-Hispanic white men (38.6 cases per 100,000 people) and non-Hispanic white women (25.5 cases per 100,000 people).2 Most patients (66.2%) are diagnosed between the ages of 55 and 84 (median age at diagnosis, 65 years), the median age at death is 71 years, and the overall death rate is 2.2 per 100,000 people per year.2 In the past decade (2010-2019), a 1.2% increase in incidence rates but a 3.2% decrease in mortality rates have been noted, which may indicate improvements in both screening and treatment.2
Up to 47% of primary melanomas and 55% of metastatic melanomas have mutations in the B-raf proto-oncogene, serine/threonine kinase (BRAF), and the 2 most common mutations are BRAF V600E and V600K.4,5 Without treatment with a BRAF inhibitor, patients with BRAF mutations have a significantly lower median overall survival (OS) compared with those with wild-type BRAF (11.1 months vs 46.1 months, respectively; P = .006), corresponding to a 23% higher relative mortality risk.4,6 Specifically, the BRAF V600E mutation is associated with a relative mortality risk that is 1.7 times higher than that of wild-type BRAF.6
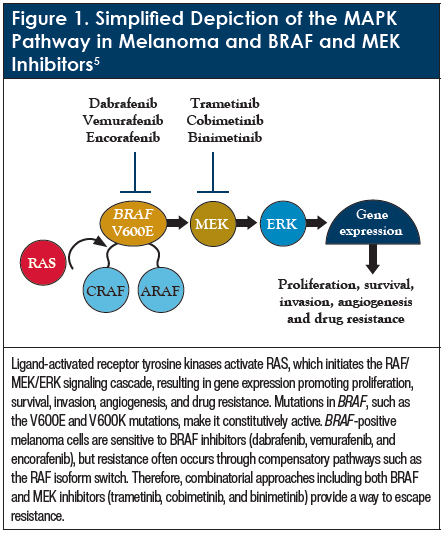
Targeted therapies that focus on the mitogen-activated protein kinase (MAPK) pathway, specifically BRAF inhibitors (dabrafenib, vemurafenib, and encorafenib) and MEK inhibitors (trametinib, cobimetinib, and binimetinib), have shown success in the treatment of BRAF-positive melanomas.7,8 Treatment with combinations of BRAF and MEK inhibitors, such as dabrafenib plus trametinib, the first approved combination in the metastatic setting and the only approved combination in the adjuvant setting, are more beneficial than monotherapy regimens.8,9 Other combinations include vemurafenib plus cobimetinib and encorafenib plus binimetinib.8 These combination regimens have lower rates of treatment-resistant disease, leading to longer progression-free survival (PFS) and OS, response rates >60%, and complete response rates between 10% and 18%; thus, these combination agents are now the standard of care for targeted therapy in patients with melanoma.7-9
Combination BRAF/MEK inhibitor therapies are associated with adverse events (AEs) that can be challenging to manage, however.10 In particular, the combination of dabrafenib plus trametinib is associated with pyrexia, which led to drug discontinuation in 8.7% of participants in the COMBI-AD trial.11,12 Recently, results from the COMBI-APlus clinical trial that used a new pyrexia management algorithm showed reduced incidence of severe pyrexia, which helped patients remain on therapy.12
This article will review pivotal clinical trials using the dabrafenib plus trametinib combination and a new protocol for management of pyrexia in patients taking this combination. Additional discussions and commentary offer practical advice to clinical pharmacists to promote long-term treatment adherence and overcome barriers to therapy, which will aid in bridging the gap between clinical trials and clinical practice.
Commentary by Paul Forsberg, PharmD, MHA, BCOP: Targeted BRAF and MEK inhibitors have improved the treatment options, outcomes, and toxicity profiles for patients with metastatic melanoma. As we have seen with other diseases, having a targetable mutation for which we have actionable drugs has improved our ability to manage these diseases. When BRAF inhibitors were first approved, patients generally had good overall response rates, but we also saw relapses. The combination of BRAF and MEK inhibitors has helped prevent resistance and improve outcomes in these patient populations. I believe the COMBI trials were key in showing the benefit of the combination regimen.
Commentary by Sanjiv Agarwala, MD: We finally have effective treatments for metastatic melanoma, which we never had before. The treatment landscape started with single-agent immunotherapies, then targeted agents, followed by combinations; and now we have targeted agents for the MAPK pathway, with BRAF/MEK combinations becoming the standard. Nowadays, we obtain a BRAF mutation test as quickly as possible for every patient with melanoma. If the patient has metastatic melanoma and wild-type BRAF, we cannot use targeted therapy, so we use immunotherapy. If the tumor has a BRAF mutation, we can choose from among the 3 approved BRAF/MEK combinations or immunotherapy. In the adjuvant setting, the choices are either a programmed death 1 inhibitor alone or dabrafenib/trametinib, which is the only approved combination treatment.
Overview of the MAPK Pathway and the Role of BRAF and MEK Inhibitors in Patients with High-Risk Resected or Metastatic Melanoma
The MAPK pathway has a key role in modulating survival, proliferation, invasion, and angiogenesis in melanoma.5 Figure 1 shows a simplified diagram of the MAPK signaling pathway starting with ligand-activated membrane-bound receptors, which then transmit the signal via the RAS/RAF/MEK/ERK axis leading to gene expression that promotes expansion.5 The most frequent mutations found in patient samples are BRAF mutations: V600E represents approximately 80% of all BRAF mutations, followed by V600K at approximately 16%.5 Although MEK mutations are not common in melanoma, MEK inhibitors do contribute to stopping the permanent activation of the MAPK pathway in these cells.5 Various studies have shown that combination BRAF/MEK inhibitor therapies are associated with superior OS, PFS, overall response rate, and duration of response, compared with monotherapy with BRAF inhibitors and are now the standard of care for targeted therapy in patients with melanoma.8,10,13-15
Commentary by Paul Forsberg, PharmD, BCOP, MHA: Having a targetable mutation, or a known biomarker, for which you have a targeted drug is a real advantage. When you have a patient with a BRAF mutation and an approved combination medication is available, as with dabrafenib plus trametinib, you can move forward with an effective treatment. Another advantage of the dabrafenib plus trametinib combination is that it has approval in the adjuvant and the metastatic settings, whereas some of the other BRAF/MEK combinations are only approved in the metastatic setting.
If treatment eventually fails, or the patient cannot tolerate it, then immune checkpoint inhibitors or another treatment are options. My perspective is that when a targetable mutation is found, you should target that first and then move on to immunotherapy.
Clinical Data in the Adjuvant Setting: COMBI-AD Study
COMBI-AD was a randomized, placebo-controlled, double-blind, phase 3 trial aimed to test the effectiveness of the dabrafenib/trametinib combination in 870 patients with stage III melanoma with a BRAF V600E (91% of patients) or BRAF V600K (9% of patients) mutation after complete surgical resection.16 Patients were randomly assigned 1:1 to combination therapy (150 mg dabrafenib twice daily plus 2 mg trametinib once daily) or to placebo for 12 months and stratified according to their BRAF mutation status and disease stage.16 The treatment arms were well-balanced in terms of patient characteristics, and most patients had stage IIIB (41%) or stage IIIC (40%) disease.16 The primary end point was relapse-free survival (RFS), and secondary end points included OS, distant metastasis-free survival, freedom from relapse, and safety.16
At a median follow-up of 60 months, 63% of the patients in the treatment arm remained in follow-up; and at median follow-up of 58 months, 54% of patients in the placebo arm remained in follow-up.9 The median RFS had not been reached in the treatment arm compared with 16.6 months in the placebo arm (hazard ratio [HR] for relapse or death, 0.51; 95% confidence interval [CI], 0.42-0.61), and 52% of patients in the treatment arm compared with 36% in the placebo arm were alive without relapse at year 5. The percentage of patients alive at year 5 without distant metastasis was 65% and 54% in the treatment and placebo arms, respectively (HR for distant metastasis or death, 0.55; 95% CI, 0.44-0.70).9 The number of protocol-specified events to calculate OS had not yet been reached.9 However, the estimated OS rate at the 3-year follow-up was 86% in the treatment arm compared with 77% in the placebo arm (HR for death, 0.57; 95% CI, 0.42-0.79; P = .0006).16
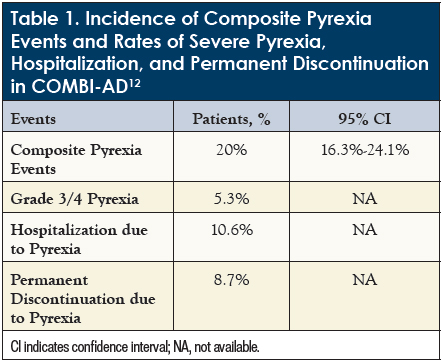
Almost all patients experienced ≥1 AEs (97% in the treatment arm, 88% in the placebo arm).16 The most common AEs were pyrexia (oral temperature of ≥38.5°C),17 fatigue, and nausea, and serious AEs (SAEs) occurred in 36% and 10% of patients in the treatment and placebo arms, respectively.16 In the treatment arm, 66% had AEs leading to dose interruptions, 38% had dose reductions, and 26% discontinued therapy, compared with 15%, 3%, and 3%, respectively, in the placebo group.16 Importantly, the rate of discontinuation due to pyrexia in the treatment arm was 8.7% (Table 1).12
Commentary by Paul Forsberg, PharmD, MHA, BCOP: The main takeaway from the COMBI-AD trial is that targeting the BRAF mutation in the adjuvant setting resulted in improved estimated OS rates at the 3-year follow-up, compared with placebo. This is really promising, because although a lot of patients are diagnosed at stage IV, many patients are diagnosed earlier. The question is whether it would be of clinical benefit to target BRAF mutations in earlier-stage disease. This trial demonstrated that significant OS improvement can occur in stage III disease utilizing targeted BRAF/MEK treatment. Another key aspect is that pyrexia led to a significant discontinuation rate, which was concerning, but it generated an opportunity for further investigation as to how to manage pyrexia and prevent discontinuations.
Clinical Data: Strategies for Managing Pyrexia in the COMBI-APlus Study
Pyrexia, without clinical or microbial evidence of infection, was the most common adverse reaction observed in the COMBI-AD trial of dabrafenib/trametinib combination in the adjuvant setting: 63% of patients experienced any grade pyrexia and 5% had grade 3/4 SAEs.12,16 Furthermore, pyrexia led to discontinuation of treatment in 8.7% of patients.12
A higher rate of pyrexia in the combination arm was also reported in the COMBI-d trial in the dabrafenib/trametinib combination arm compared with the dabrafenib monotherapy arm (51% and 28%, respectively), indicating that trametinib is probably involved in the process leading to the emergence of pyrexia.12,13,17 If pyrexia syndrome is not managed appropriately, it has the potential to worsen over time resulting in dehydration, leading to hypotension and associated organ damage.18,19 Severe/complicated pyrexia syndrome may require hospitalization and can have a negative impact on patient quality of life and expose patients to hospital-acquired infections and increased healthcare costs.12,20
At the 5-year analysis of the COMBI-AD trial, 52% of the patients in the combination group were alive without relapse, compared with only 36% in the placebo group, indicating the benefit of this treatment in increasing survivorship in patients with high-risk resected melanoma. Improved pyrexia management, however, could result in a better outcome for patients and allow more patients to complete the 12-month treatment regimen.9,12
The cause of dabrafenib/trametinib-related pyrexia is not well-understood, and no associations have been found between patient or disease characteristics and pyrexia. Therefore, it is not possible to predict which patients will experience pyrexia or the severity of the pyrexia before starting treatment.17,18 A few updated strategies for managing pyrexia in patients receiving dabrafenib/trametinib combination therapy have been published.10,18,19,21 However, consistency was lacking as to strategies used in the management of treatment-related pyrexia in patients taking dabrafenib/trametinib.
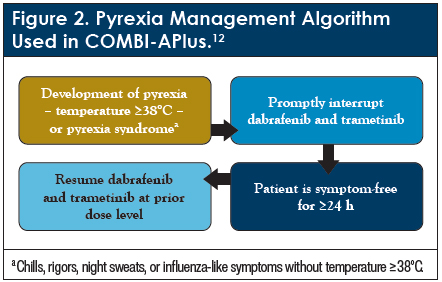
Thus, the COMBI-APlus clinical trial was initiated to investigate whether a modified pyrexia management algorithm (Figure 2) could result in fewer occurrences of serious pyrexia-related AEs, including hospitalizations and treatment discontinuations.12 The COMBI-APlus study was an open-label, multicenter, phase 3b study. To be eligible, patients had to be aged ≥18 years with completely resected BRAF V600E or V600K mutation–positive stage III melanoma. Patients received the same dosage as patients in the COMBI-AD trial (150 mg dabrafenib twice daily plus 2 mg trametinib once daily) for 12 months or until discontinuation, followed by a 12-month follow-up period. All patients who developed pyrexia were treated according to the new pyrexia management algorithm and results were compared with the historical control from COMBI-AD. The primary end point of this study was the composite rate of severe (grade 3/4) pyrexia, compared with the rate seen in COMBI-AD. Secondary end points included RFS and safety.12
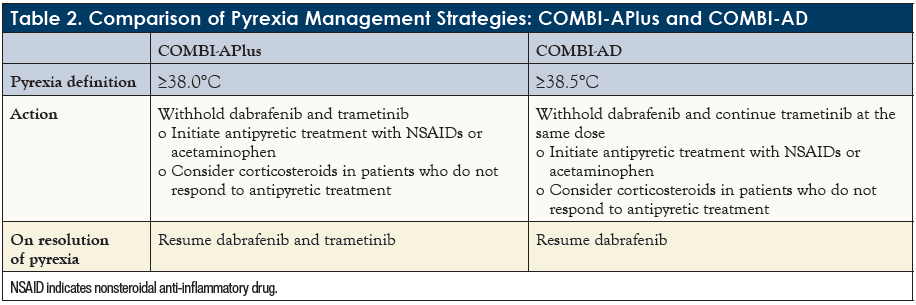
The modified pyrexia management algorithm included a new definition of pyrexia with a lower temperature threshold (≥38°C vs ≥38.5°C), as well as a new definition of pyrexia syndrome (chills, rigors, night sweats, or influenza-like symptoms without elevated temperature). Both dabrafenib and trametinib were interrupted promptly upon development of pyrexia or pyrexia syndrome and were resumed at the prior dose level following 24 hours of no pyrexia symptoms. Antipyretic treatment and, for patients whose fever does not resolve with antipyretics, corticosteroids were also recommended (Table 2).12
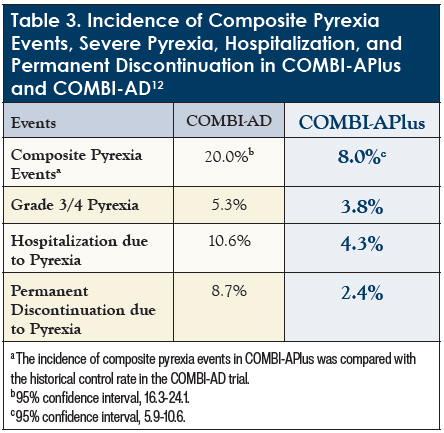
As shown in Table 3, the composite rate of severe pyrexia was 8.0% (95% CI, 5.9%-10.6%) in the COMBI-APlus study, compared with 20.0% in COMBI-AD.12 In the COMBI-APlus trial, there were 2068 on-treatment pyrexia events (all grades), corresponding to 67.8% of patients. The median time to first onset of pyrexia was 22 days (interquartile [IQR] range, 11-69 days), and pyrexia events had a median duration of 2.0 days (IQR, 2.0-4.0 days). Among patients who experienced pyrexia, 51.9% had grade 1, 42.5% had grade 2, 4.0% had grade 3, and 1.6% had grade 4 events, showing that most events were low grade (1 or 2). Some pyrexia events led to dose interruptions or reductions; there were 61.6% dose interruptions and 5.8% dose reductions for dabrafenib, and 60.9% and 4.3% for trametinib, respectively.12 These results indicate that there was a significant reduction in composite pyrexia events using the modified pyrexia regimen in COMBI-APlus, compared with the COMBI-AD trial.12
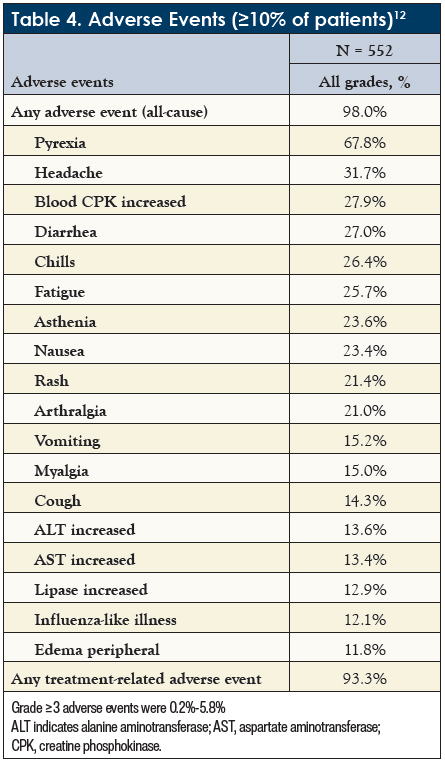
In the COMBI-APlus trial, almost all patients (98.0%) experienced AEs (Table 4) and 40.9% experienced SAEs (grade ≥3); AEs resulted in discontinuation of both drugs in 14.7%.12 Overall, the safety profile was similar to that of the COMBI-AD study, indicating that the new algorithm mainly affects the composite rate of pyrexia.12
In the COMBI-APlus trial, the median duration of treatment for both dabrafenib and trametinib was 11.0 months, with a median relative dose intensity of 94.5%, and the RFS at 12 months was 91.8% (95% CI, 89.0%-93.9%); these results were comparable to findings in the COMBI-AD study.12,16
Of note, fewer treatment discontinuations occurred in COMBI-APlus versus COMBI-AD, indicating that the new pyrexia management algorithm resulted in greater treatment tolerability.12 Thus, the prescribing information for dabrafenib and trametinib was updated in 2021 to include the pyrexia management algorithm described in COMBI-APlus. For information about dosing, dose reductions, and dose modifications due to common AEs, healthcare providers can consult the prescribing information documents for both drugs.11,22
Commentary by Paul Forsberg, PharmD, MHA, BCOP: A key takeaway from the COMBI-APlus trial is that it validated an approach that includes providing early patient education, identifying toxicities earlier, and giving patients tools and supportive care (such as nonsteroidal anti-inflammatory drugs or acetaminophen) earlier on to manage pyrexia. This patient-centered approach helped reduce the incident rate and severity of pyrexia. The incidence of grade 3 AEs associated with pyrexia was lower in COMBI-APlus, which ultimately resulted in fewer hospitalizations and treatment discontinuations, which is our ultimate goal. We want to intervene so that patients can stay on therapy longer.
Historically, some of the standards for what constitutes a fever might have been higher than what you see in patients, so lowering the threshold for what triggered pyrexia identification helped with earlier management and the prevention of severe disease. In addition, it is important to know that both the BRAF and MEK inhibitors can lead to pyrexia and that there seems to be a synergistic effect between the 2 agents, and suspending both drugs helped manage pyrexia.
With many drugs, we see toxicities and then create a plan to help get patients through them. Having the COMBI-APlus clinical trial data and a toxicity management algorithm support the approach that we would take in this patient population. Thus, COMBI-APlus has significantly improved patient interactions with the pharmacy team and with education materials and has provided important tools to help improve patient adherence.
Commentary by Sanjiv Agarwala, MD: The COMBI-APlus trial was a very good addition to our knowledge base of pyrexia and its management. Pyrexia can result in discontinuation of treatment. The takeaway from the COMBI-APlus trial is that this adapted pyrexia management algorithm is effective and helps reduce grade 3/4 fevers, hospitalizations, and treatment discontinuation. This new approach should be put into practice so oncologists can adopt it to help aid adherence with the regimen. I thought these results were very important given that dabrafenib/trametinib is the only approved combination in the adjuvant setting and that these are the patients who we should be most careful about, ensuring adequate quality of life and providing efficacious therapy without having to admit the patient to a hospital due to fever.
I had been using this kind of algorithm even before the results came out and have been using it even more since, and I find that it does make a difference. Now, when we start somebody on this combination therapy, we spend a lot more time talking about pyrexia in addition to the other AEs. We tell patients what we are going to do and how closely we are going to monitor it, to call us at the first sign of a fever so we can treat them early and follow the algorithm. We have a team that is dedicated to seeing these patients on a regular schedule if they do not call us.
The difference between how COMBI-AD and COMBI-APlus managed pyrexia is that the new algorithm is very systematic and rigorous. The decision to stop both drugs, compared to a debate about which drug to stop or reduce, is clear. I think we might need to be more rigorous about the 0.5-degree change in the definition of pyrexia, but this represents a more systematic implementation of something that we already knew.
The Role of Oncology Pharmacists
Oncology pharmacists are important participants in the multidisciplinary approach to optimize the treatment of patients with BRAF-positive melanoma. Pharmacists play various roles23:
- Prescription validation: verify that the treatment choice falls within the clinical indication for the prescribed drugs, determine appropriate dosage considering the patient’s hepatic and renal function
- Medication reconciliation: take into account any complementary/alternative therapies to determine and manage potential drug interactions
- Treatment preparation: must be done safely and in accordance with the current guidelines for manipulation of hazardous products and recommendations for basic aseptic technique
- Education for both healthcare professionals and patients: oncology pharmacists typically meet with each patient to explain the chosen treatment; information should be provided to patients in a written handout that includes clear contact information for any questions, issues, or worries
- AE management and supportive care: how to prevent, recognize, and/or control AEs
Electronic health records (EHRs) include records from other providers and past visits, laboratory values, images, and progress notes. They can also include information that supports medical decisions, such as clinical guidelines or best medical practices and algorithms that check for drug interactions. EHRs provide many advantages, including increased search capabilities, automated reminders, improved information sharing, and increased transparency.24 EHRs can affect patient safety and clinical outcomes in a variety of ways; for example, identifying and preventing errors (checking for drug allergies, drug interactions, and dosing errors), minimizing deviations from best practices with prespecified order sets, improving clinical communication and coordination across multidisciplinary teams, improving information management for patients (multiple comorbidities, and extensive monitoring and testing), and reducing fragmentation of care.24 For patients with melanoma, EHRs can help identify high-risk patients who are due for screening tests, leading to earlier detection of recurrent disease and increased patient survival.25
Commentary by Paul Forsberg, PharmD, MHA, BCOP: With any new patient starting on an oral agent or with a new diagnosis of BRAF-positive melanoma, our pharmacists do a thorough clinical review. They will ensure that patients have the right drug for the right disease and that the mutation has been documented through appropriate testing and confirmed by pathology reports. Then they will verify that the dosing and treatment is correct, based on clinical pathways and treatment algorithms. Following that, they will look for significant drug interactions. We know that there is a potential risk of drug interactions with dabrafenib and trametinib, which can create an increased risk of toxicities. They also analyze if any dosing adjustments may be necessary for a patient, based on their hepatic function.
Following the clinical review, pharmacists educate the patient. Of note, with the combination of dabrafenib/trametinib, pharmacists will discuss potential toxicities, when to expect them, and if an AE does occur, how to manage it. This is particularly true for toxicities that we try to prevent and manage earlier, such as in those patients with a higher risk profile or higher incidence of grade 3 events. In this case, the data from the COMBI-APlus trial give pharmacists and patients the tools to help identify and intervene in pyrexia earlier.
Pharmacists meet with patients and educate them prior to treatment initiation. They also inquire about AEs when refilling medications. We use the Oral Chemotherapy Education sheets, developed through a joint venture through the American Society of Clinical Oncology, the National Community Oncology Dispensing Association, and the Oncology Nursing Society; these have been a way to standardize patient education. These education sheets include information around monitoring for pyrexia when starting treatment for melanoma.
In the world of oncology drug development, we used to see 3 to 5 new indications a year and provide specific education to clinicians and pharmacists around that. Now there are 60 to 65 new US Food and Drug Administration (FDA) approvals annually in the hematology/oncology arena. Thus, it is difficult to stay on top of all the latest evidence and indications, and it is important, from a system level, that we have standardized tools and education materials. When we see significant changes in the way we deploy treatments, we try to educate our providers as soon as possible so the tools are available when identifying and ordering a treatment for a patient.
The Clinical Pathway Program we use integrates with the EHR systems, and it plays a key role in standardizing care. We use the Clear Value Plus, which is a US Oncology program. Basically, the practitioner will enter the disease, stage, and any biomarkers or mutations that the patient might have into the system. Then, the algorithm identifies appropriate treatments based on this information. Ideally, EHR systems would allow for laboratory results to be included with the orders and integrate more hard stops for biomarker testing and evaluation prior to starting treatment. This would ensure that we use the best treatment, correct dose, and correct supportive care, based on current clinical evidence. For example, ensuring that the correct supportive care medications are built into the protocols so that patients receive optimal management of those AEs when needed. Finally, because it is difficult to remain abreast of new evidence, the system helps guarantee that staff are using up-to-date clinical resources, such as the package inserts with updated dosing and information on AE management and the management information stemming from the COMBI-APlus trial.
The COMBI-APlus trial demonstrated that a multidisciplinary team can improve patient outcomes by keeping them on treatment longer. Ensuring that a patient receives the medication and stays on it longer gives the best chance of getting a durable response.
Commentary by Sanjiv Agarwala, MD: In our practice, most of the communication with the patient comes from our nurses and our clinical team. We inform the clinical pharmacist to be alert for changes in prescriptions or AE management to verify that they are a good fit for the patient and to alert us about any issues. Clinical pharmacists are more involved in this aspect in our practice. One issue is that many of my patients are located at great distance and use different pharmacies to obtain their drugs, so we are attacking AE management at the source, when the drug is being prescribed.
The challenge with oral drugs is that information does not come from a single source. You need the prescriber or nurse to talk to the patient about how to take the drug and manage AEs.
The main change I have made recently in treating patients with metastatic melanoma involves choosing the targeted therapy that we can tailor to the patient as far as possible. I follow this improved algorithm, and I have had better adherence and overall improved outcomes with targeted therapy. The COMBI-APlus trial has helped in terms of managing patients better.
I think that the COMBI-APlus algorithm is especially important in the adjuvant space because these are patients who are healthy and technically cured. Making sure that their quality of life is the best possible and that they can continue with their regular daily activities and jobs if they are employed is extremely important. These are the patients who are most likely to be nonadherent with the medications if they experience a deterioration in their quality of life because unlike metastatic patients, they are not seeing any visible benefit from the therapy. The take-home message for me is to be very aggressive in managing patients in the adjuvant setting because once they walk away, if they have a bad experience, they will not want to be treated again. They will say, “I could have chosen not to take treatment, but I took it and because I had this bad AE, I don’t think I’m going to go back on it.” We must be very careful when applying the COMBI-APlus algorithm.
Conclusion
The introduction of targeted therapies, such as the combination of dabrafenib plus trametinib, for the treatment of metastatic melanoma with BRAF V600E or V600K mutations has resulted in a substantial increase in survival in recent years. Durable disease control and even cure are now possible for patients with metastatic melanoma, which was uncommon a decade ago. In addition, these therapies are successful in the adjuvant and neoadjuvant settings.
The first FDA-approved targeted combination therapy is dabrafenib plus trametinib. This combination has been shown to result in an estimated 12-month RFS rate of 88% in the adjuvant setting (COMBI-AD). However, 8.7% of the patients in that study stopped therapy due to treatment-related pyrexia. The COMBI-APlus trial tested a new pyrexia management algorithm, which lowered the treatment discontinuation rate due to pyrexia to 2.5%, with a comparable 12-month RFS rate of 92%.
Physicians and clinical pharmacists play an important role in ensuring that patients adhere to treatment with combination dabrafenib/trametinib. Before beginning treatment, physicians and clinical pharmacists do a thorough clinical review to ensure that the treatment choice and dosage are appropriate for the patient considering disease-specific factors, comorbidities, and other prescription medications. Furthermore, healthcare practitioners play a critical role in educating patients about the importance of taking the medication as prescribed and how to monitor for and manage pyrexia early before it becomes serious and requires hospitalization. This education is especially important with oral medications such as dabrafenib and trametinib. The use of EHRs helps standardize clinical practice in terms of diagnostic criteria, treatment decisions, patient education, and management of AEs such as pyrexia.
References
- American Cancer Society. Cancer facts & figures 2022. www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2022/2022-cancer-facts-and-figures.pdf. Accessed April 29, 2022.
- National Cancer Institute. Cancer stat facts: melanoma of the skin. seer.cancer.gov/statfacts/html/melan.html. Accessed April 28, 2022.
- Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022;72(1):7-33.
- Long GV, Menzies AM, Nagrial AM, et al. Prognostic and clinicopathologic associations of oncogenic BRAF in metastatic melanoma. J Clin Oncol. 2011;29(10):1239-1246.
- Vultur A, Villanueva J, Herlyn M. Targeting BRAF in advanced melanoma: a first step toward manageable disease. Clin Cancer Res. 2011;17(7):1658-1663.
- Ny L, Hernberg M, Nyakas M, et al. BRAF mutational status as a prognostic marker for survival in malignant melanoma: a systematic review and meta-analysis. Acta Oncol. 2020;59(7):833-844.
- Eddy K, Chen S. Overcoming immune evasion in melanoma. Int J Mol Sci. 2020;21(23):8984-9031.
- Curti BD, Faries MB. Recent advances in the treatment of melanoma. N Engl J Med. 2021;384(23):2229-2240.
- Dummer R, Hauschild A, Santinami M, et al. Five-year analysis of adjuvant dabrafenib plus trametinib in stage III melanoma. N Engl J Med. 2020;383(12):1139-1148.
- Czupryn M, Cisneros J. BRAF/MEK inhibitor therapy: consensus statement from the faculty of the melanoma nursing initiative on managing adverse events and potential drug interactions. Clin J Oncol Nurs. 2017;21(4 Suppl):11-29.
- Mekinist. Mekinist (trametinib) prescribing information. www.novartis.us/sites/www.novartis.us/files/mekinist.pdf. Accessed May 6, 2022.
- Atkinson V, Robert C, Grob JJ, et al. Improved pyrexia-related outcomes associated with an adapted pyrexia adverse event management algorithm in patients treated with adjuvant dabrafenib plus trametinib: primary results of COMBI-APlus. Eur J Cancer. 2022;163:79-87.
- Long GV, Stroyakovskiy D, Gogas H, et al. Combined BRAF and MEK inhibition versus BRAF inhibition alone in melanoma. N Engl J Med. 2014;371(20):1877-1888.
- Robert C, Karaszewska B, Schachter J, et al. Improved overall survival in melanoma with combined dabrafenib and trametinib. N Engl J Med. 2015;372(1):30-39.
- Larkin J, Ascierto PA, Dréno B, et al. Combined vemurafenib and cobimetinib in BRAF-mutated melanoma. N Engl J Med. 2014;371(20):1867-1876.
- Long GV, Hauschild A, Santinami M, et al. Adjuvant dabrafenib plus trametinib in stage III BRAF-mutated melanoma. N Engl J Med. 2017;377(19):1813-1823.
- Menzies AM, Ashworth MT, Swann S, et al. Characteristics of pyrexia in BRAFV600E/K metastatic melanoma patients treated with combined dabrafenib and trametinib in a phase I/II clinical trial. Ann Oncol. 2015;26(2):415-421.
- Atkinson V, Long GV, Menzies AM, et al. Optimizing combination dabrafenib and trametinib therapy in BRAF mutation-positive advanced melanoma patients: guidelines from Australian melanoma medical oncologists. Asia Pac J Clin Oncol. 2016;12(Suppl 7):5-12.
- Thawer A, Miller WH Jr, Gregorio N, et al. Management of pyrexia associated with the combination of dabrafenib and trametinib: Canadian consensus statements. Curr Oncol. 2021;28(5):3537-3553.
- Guy GP Jr, Ekwueme DU, Tangka FK, Richardson LC. Melanoma treatment costs: a systematic review of the literature, 1990-2011. Am J Prev Med. 2012;43(5):537-545.
- Daud A, Tsai K. Management of treatment-related adverse events with agents targeting the MAPK pathway in patients with metastatic melanoma. Oncologist. 2017;22(7):823-833.
- Tafinlar. Tafinlar (dabrafenib) prescribing information. www.novartis.us/sites/www.novartis.us/files/tafinlar.pdf. Accessed May 6, 2022.
- Gazzé G. Combination therapy for metastatic melanoma: a pharmacist’s role, drug interactions & complementary alternative therapies. Melanoma Manag. 2018;5(2):MMT07.
- Atasoy H, Greenwood BN, McCullough JS. The digitization of patient care: a review of the effects of electronic health records on health care quality and utilization. Annu Rev Public Health. 2019;40:487-500.
- Reisenauer A, Lee BJ, Akamine K, Tabacchini M, Golden S. Management of melanoma in a patient population: using electronic health records to enhance postdiagnosis surveillance. JAMA Dermatol. 2013;149(3):365-366.