Lung and bronchus cancer, the second most common form of cancer, accounts for 13.5% of all new cancer cases in the United States.1 In 2018 alone, lung cancer was newly diagnosed in 234,030 individuals and accounted for 154,050 deaths.1 In fact, lung cancer is the leading cause of cancer-related mortality in men and women, and is responsible for more than 25% of all cancer deaths. The 5-year survival rate for patients whose lung cancer has spread regionally (to regional lymph nodes) is 29.7%, but that survival rate is only 4.7% for patients with distant metastases.1
US healthcare costs associated with lung cancer impose a substantial economic burden, accounting for $13.9 billion in 2017.2 Of this total, $6 billion was for initial care, $5.8 billion was for the last year of life, and $2.1 billion was for continuing care.2
The 2 main types of lung cancer are non–small-cell lung cancer (NSCLC), which accounts for 80% to 85% of all cases, and small-cell lung cancer, accounting for 10% to 15% of lung cancers.3 Mutations in the anaplastic lymphoma kinase (ALK) gene are present in approximately 5% of patients with NSCLC.4,5
The treatments for metastatic NSCLC include chemotherapy, targeted therapy, immunotherapy, or a combination of these options. For patients with NSCLC and ALK rearrangements, the first-line ALK-targeted therapies include crizotinib (Xalkori), alectinib (Alecensa), ceritinib (Zykadia), and brigatinib (Alunbrig), which was initially approved only as a second-line therapy.4,5
Lorbrena Approved for ALK-Positive Metastatic NSCLC
On November 2, 2018, lorlatinib (Lorbrena; Pfizer) was approved by the US Food and Drug Administration (FDA) for the treatment of patients with ALK-positive metastatic NSCLC whose disease progressed after receiving crizotinib and at least 1 other ALK inhibitor for metastatic disease, or for those whose disease progressed after alectinib or ceritinib treatment as the first ALK inhibitor for metastatic disease.6,7
Lorlatinib, an oral kinase inhibitor, was granted accelerated approval for this indication by the FDA based on tumor response rate and duration of response in a subgroup of patients with ALK-positive metastatic NSCLC in a phase 2 clinical trial.8 The continued approval of lorlatinib may be subject to verification of its clinical benefit in a confirmatory trial.7
Mechanism of Action
Lorlatinib is a kinase inhibitor that has shown in vitro activity against several genes and protein rearrangements, including ALK, ROS1, TYK1, FER, FPS, TRKA, TRKB, TRKC, FAK, FAK2, and ACK.7 Moreover, lorlatinib has shown activity against multiple alterations of the ALK enzyme, including tumor mutations developed during disease progression after receiving crizotinib or other ALK inhibitors. In preclinical studies, the antitumor activity of lorlatinib was dose-dependent and correlated with the inhibition of ALK phosphorylation.7
Dosing and Administration
Lorlatinib is available as 25-mg or 100-mg tablets for oral use.7 The recommended dose of lorlatinib is 100 mg orally once daily, taken at the same time every day, with or without food. If lorlatinib tablets are broken or cracked, they should not be ingested; the tablets should be swallowed whole and should not be chewed, crushed, or split.7
Pivotal Clinical Trial
The safety of lorlatinib was evaluated in a cohort of 215 patients with ALK-positive metastatic NSCLC who received previous treatment with 1 or more ALK kinase inhibitors in the nonrandomized, multicohort, multicenter phase 2 clinical trial, Study B7461001, that included a total of 332 patients.7,8 The primary efficacy end points were overall response rate and intracranial overall response rate, according to Response Evaluation Criteria in Solid Tumors (RECIST) version 1.1, as assessed by an Independent Central Review committee.
The data were pooled across several patient subgroups, based on the history of previous therapy, including previous crizotinib therapy and no chemotherapy; previous crizotinib and 1 to 2 lines of chemotherapy; previous ALK inhibitor (other than crizotinib), with or without chemotherapy; 2 previous ALK inhibitors, with or without chemotherapy; and 3 previous ALK inhibitors, with or without chemotherapy.
Of the cohort of 215 patients enrolled in the study, the median age was 53 years and 95% had the adenocarcinoma subtype of NSCLC.7
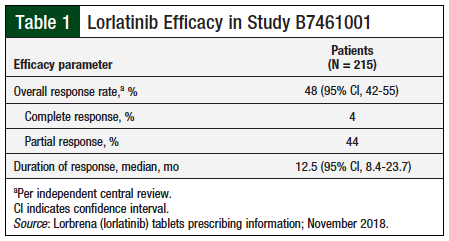
Overall, 48% of patients who received treatment with lorlatinib achieved an overall response, and the median duration of response was more than 1 year (Table 1).7 Notably, the majority of patients who achieved an overall response with lorlatinib had disease progression after receiving 3 or more ALK-targeted treatments, including the second-generation ALK tyrosine kinase inhibitors alectinib, ceritinib, and brigatinib.8 Moreover, 60% of patients who received lorlatinib and had measurable lesions in the central nervous system ([CNS] according to RECIST version 1.1) had an intracranial response, with a median response duration of more than 1.6 years (Table 2).7
An ongoing phase 3 clinical trial called CROWN is comparing the efficacy of first-line treatment with lorlatinib versus crizotinib in prolonging progression-free survival and overall survival in patients with advanced ALK-positive NSCLC.9
Adverse Reactions
Of 295 patients who received 100 mg of lorlatinib orally once daily in Study B7461001, the most common (incidence ≥20%) adverse reactions associated with lorlatinib were edema (57%), peripheral neuropathy (47%), cognitive effects (27%), dyspnea (27%), fatigue (26%), weight gain (24%), arthralgia (23%), mood effects (23%), and diarrhea (22%).
Serious adverse events were reported in 32% of the 295 patients; the most common were pneumonia (3.4%), dyspnea (2.7%), pyrexia (2%), mental status changes (1.4%), and respiratory failure (1.4%). Fatal adverse reactions occurred in 2.7% of the patients.7
Overall, 8% of patients permanently discontinued lorlatinib treatment; the most common adverse reactions leading to discontinuation were respiratory failure (1.4%), dyspnea (0.7%), myocardial infarction (0.7%), cognitive effects (0.7%), and mood effects (0.7%).7
Contraindications
Lorlatinib is contraindicated for concomitant use with strong cytochrome (CY) P3A inducers (ie, rifampin), because of the potential for hepatotoxicity.7
Drug Interactions
The concomitant use of lorlatinib with strong or moderate CYP3A inducers should be avoided.7
Lorlatinib should not be used concomitantly with strong CYP3A inhibitors, because concomitant use may increase the incidence and severity of lorlatinib-associated adverse reactions.7
Lorlatinib can decrease the concentration of CYP3A substrates when both drugs are used concomitantly; lorlatinib should not be used concomitantly with CYP3A substrates in situations where minimal concentration changes may lead to serious therapeutic failures.7
Use in Specific Populations
Women should not breastfeed during lorlatinib treatment and for 7 days after the final dose because of the risk for serious adverse reactions in breastfed infants.7
Data are limited on the use of lorlatinib in patients aged ≥65 years; in Study B7461001, 18% of the 295 patients who were exposed to lorlatinib were aged ≥65 years; no overall differences were observed between these patients and younger patients.7
No dose adjustment is needed for patients with mild hepatic impairment or those with mild or moderate renal impairment. A recommended dose has not been established for patients with moderate or severe hepatic impairment or patients with severe renal impairment.7
Warnings and Precautions
These warnings reflect data from 332 patients who were exposed to lorlatinib in the study. The concomitant use of strong CYP3A inducers with lorlatinib is associated with a risk for severe hepatotoxicity and should be avoided. Before initiating lorlatinib treatment, strong CYP3A inducers should be discontinued for 3 plasma half-lives.7
Lorlatinib is associated with CNS effects, including seizures, hallucinations, and changes in cognitive function, mood, speech, mental status, and sleep patterns. Depending on the severity of these effects, lorlatinib should be withheld and resumed at the same dose or at a reduced dose, or permanently discontinued.7
Increases in serum cholesterol and triglycerides can occur with lorlatinib treatment. In patients with hyperlipidemia, lipid-lowering agents should be initiated or their dose increased. Serum cholesterol and triglycerides should be monitored before initiating treatment with lorlatinib; at 1 and 2 months after initiating lorlatinib treatment; and periodically thereafter. At the first hyperlipidemia event, lorlatinib should be withheld, and then resumed at the same dose; if hyperlipidemia recurs, lorlatinib should be resumed at the same, or at a reduced, dose, based on the hyperlipidemia severity.7
Atrioventricular block and PR interval prolongation can occur in patients who receive lorlatinib treatment. Patients should be monitored (by electrocardiogram) before starting lorlatinib therapy and periodically thereafter. For patients who undergo pacemaker placement, lorlatinib should be withheld and resumed at a reduced dose. For patients whose atrioventricular block recurs, lorlatinib treatment should be permanently discontinued.7
Interstitial lung disease or pneumonitis can occur with lorlatinib. In patients with suspected interstitial lung disease or pneumonitis, lorlatinib should be withheld. In patients with treatment-related interstitial lung disease or pneumonitis of any severity, lorlatinib should be permanently discontinued.7
Lorlatinib can cause harm to a fetus; pregnant women should be advised of this risk. Women and men of reproductive potential should use effective nonhormonal contraception during lorlatinib treatment. Women should continue to use contraception for at least 6 months after the final dose of lorlatinib, and men should continue the use of contraception for at least 3 months after the final dose.7
Conclusion
The FDA approval of lorlatinib provides a new oral treatment option for patients with metastatic NSCLC that is associated with an ALK mutation. Lorlatinib, an ALK-targeted kinase inhibitor, demonstrated a substantial overall response and intracranial response in patients with ALK-positive metastatic NSCLC whose disease progressed after receiving crizotinib and at least 1 other ALK inhibitor, or after receiving alectinib or ceritinib.7,8
References
- National Cancer Institute. SEER cancer stat facts: lung and bronchus cancer. https://seer.cancer.gov/statfacts/html/lungb.html. Accessed January 3, 2019.
- National Cancer Institute. Cancer Trends Progress Report: Financial Burden of Cancer Care. February 2018. https://progressreport.cancer.gov/after/economic_burden. Accessed January 4, 2018.
- American Cancer Society. What is non-small cell lung cancer? Revised May 16, 2016. www.cancer.org/cancer/non-small-cell-lung-cancer/about/what-is-non-small-cell-lung-cancer.html. Accessed January 3, 2019.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Non-Small Cell Lung Cancer. Version 3.2019. January 18, 2019. www.nccn.org/professionals/physician_gls/pdf/nscl.pdf. Accessed January 4, 2019.
- American Cancer Society. Targeted therapy drugs for non-small cell lung cancer. Revised November 5, 2018. www.cancer.org/cancer/non-small-cell-lung-cancer/treating/targeted-therapies.html. Accessed January 7, 2018.
- US Food and Drug Administration. FDA approves lorlatinib for second- or third-line treatment of ALK-positive metastatic NSCLC. November 2, 2018. www.fda.gov/Drugs/InformationOnDrugs/ApprovedDrugs/ucm625027.htm. Accessed December 27, 2018.
- Lorbrena (lorlatinib) tablets, for oral use [prescribing information]. New York, NY: Pfizer; November 2018.
- Solomon BJ, Besse B, Bauer TM, et al. Lorlatinib in patients with ALK-positive non-small-cell lung cancer: results from a global phase 2 study. Lancet Oncol. 2018;19:1654-1667. Erratum in: Lancet Oncol. 2019;20:e10.
- ClinicalTrials.gov. A study of lorlatinib versus crizotinib in first line treatment of patients with ALK-positive NSCLC. January 28, 2019. https://clinicaltrials.gov/ct2/show/NCT03052608. Accessed February 20, 2019.