Multiple myeloma is a cancer of plasma cells in the bone marrow that often leads to bone destruction and bone marrow failure.1,2 According to the American Cancer Society, more than 26,800 new cases of multiple myeloma were diagnosed in 2015, and 11,240 deaths were attributed to the disease.3
Representing approximately 1% of all cancer cases globally, multiple myeloma is the second most common hematologic malignancy after non-Hodgkin lymphoma.4 The incidence of multiple myeloma is higher among men than among women.1 Individuals aged ≥65 years, those with a family history of multiple myeloma, and those with a personal history of monoclonal gammopathy of undetermined significance are at an increased risk for multiple myeloma.1 Several common complications of multiple myeloma include bone pain, kidney dysfunction, bone loss, impaired immunity, and anemia.5
Although the overall incidence of multiple myeloma continues to increase, the mortality rates associated with this malignancy have declined in the past 20 years.1,6 Specifically, the advent of novel therapy options for multiple myeloma, as well as improvements in high-dose therapy and supportive care have contributed to extended survival for patients with this disease.6
New anticancer drugs and novel combinations have emerged in part thanks to improved understanding of the bone marrow microenvironment and the biology of multiple myeloma.7 Immunomodulatory drugs (IMiDs) and proteasome inhibitors now represent the cornerstones of initial treatment for multiple myeloma based on their proved ability to enhance the overall response rates and survival.2,7
Because novel agents for multiple myeloma have had a considerable impact on the healthcare budget, understanding their relative cost-effectiveness is important for ensuring their efficient use. Overall, 2 recent evaluations of the economics of these new agents in multiple myeloma resulted in similar conclusions.8,9
One of the studies used claims data from more than 2600 US-based patients with multiple myeloma, showing that the 1-year costs of bortezomib-based therapy were similar to those of non-novel combinations (approximately $112,000 each), whereas the costs of thalidomide- and lenalidomide-based regimens were significantly higher (approximately $130,500 and $159,200, respectively) than non-novel combinations.8 This study also found that patients taking thalidomide and lenalidomide had higher out-of-pocket costs in light of Medicare Part D’s coverage gap for outpatient drugs.8
The second study modeled the cost-effectiveness of novel agents combined with melphalan and prednisone in patients with newly diagnosed multiple myeloma who were ineligible for a transplantation. The researchers concluded that adding bortezomib to melphalan plus prednisone was more cost-effective than adding thalidomide or lenalidomide to that regimen.9
Despite strides in the treatment of multiple myeloma, patients will experience disease relapse after initial treatment and several lines of therapy are typically required.10 Specifically, resistance to bortezomib and to lenalidomide is being observed with increasing frequency; therefore, there remains a marked need for additional therapeutic options for patients with double-refractory multiple myeloma.11
Darzalex First Monoclonal Antibody for Multiple Myeloma
On November 16, 2015, the US Food and Drug Administration (FDA) approved the first monoclonal antibody, daratumumab (Darzalex; Janssen Biotech), for the treatment of patients with multiple myeloma who have received at least 3 previous lines of therapy, including a proteasome inhibitor and an IMiD, or for the treatment of patients whose disease is double-refractory to proteasome inhibitors and IMiDs.12,13 Daratumumab was approved using the FDA’s accelerated approval program, which provides early patient access to a new therapy while its developer conducts clinical trials to confirm the drug’s benefits.12
Overall, 2 open-label studies demonstrated complete or partial responses in patients with relapsed and/or refractory multiple myeloma; these studies were the basis for the FDA’s approval of daratumumab.12-15
Daratumumab targets CD38, a protein expressed on the surface of multiple myeloma cells and other hematopoietic cells.13 According to Richard Pazdur, MD, Director of the FDA’s Office of Hematology and Oncology Products, “Targeting proteins that are found on the surface of cancer cells has led to the development of important oncology treatments. Darzalex provides another treatment option for patients with MM [multiple myeloma] who have become resistant to other therapies.”12
Mechanism of Action
CD38 is a transmembrane glycoprotein that is expressed on the surface of hematopoietic cells, including multiple myeloma cells. CD38 is involved in receptor-mediated adhesion, cell signaling, and modulation of cyclase and hydrolase activity.13
Daratumumab is an immunoglobulin (Ig) G1 kappa human monoclonal antibody. After binding to CD38, daratumumab inhibits the growth of CD38-expressing tumor cells in several ways, including the induction of apoptosis directly through Fc-mediated cross-linking, induction of immune-mediated tumor-cell lysis through complement-dependent cytotoxicity, antibody-dependent cell-mediated cytotoxicity, and antibody-dependent cellular phagocytosis.13
Because CD38 is also expressed on myeloid-derived suppressor cells and on a subset of regulatory T-cells, these cells are also susceptible to daratumumab-mediated cell lysis.13
Dosing and Administration
The recommended dose of daratumumab is 16 mg/kg of body weight, administered as an intravenous infusion. Dosing is recommended according to the following schedule13:
- Weeks 1 to 8: weekly
- Weeks 9 to 24: biweekly
- Week 25+: every 4 weeks until disease progression.
To mitigate the risk for infusion reactions, patients receiving daratumumab should be premedicated with corticosteroids, antipyretics, and antihistamines. Patients should also receive corticosteroids (eg, 20 mg methylprednisolone or equivalent) on the first and second days after each daratumumab infusion to reduce the risk for delayed infusion reactions.13
Daratumumab is packaged in 100 mg/5 mL and 400 mg/20 mL single-dose vials (20 mg/mL).13
Early-Phase Clinical Trials
The efficacy and safety of daratumumab in multiple myeloma were demonstrated in the SIRIUS (MMY2002) and the GEN501 early-phase, open-label clinical trials evaluating the use of single-agent daratumumab in patients with relapsed and/or refractory multiple myeloma.13-16
The SIRIUS Clinical Trial
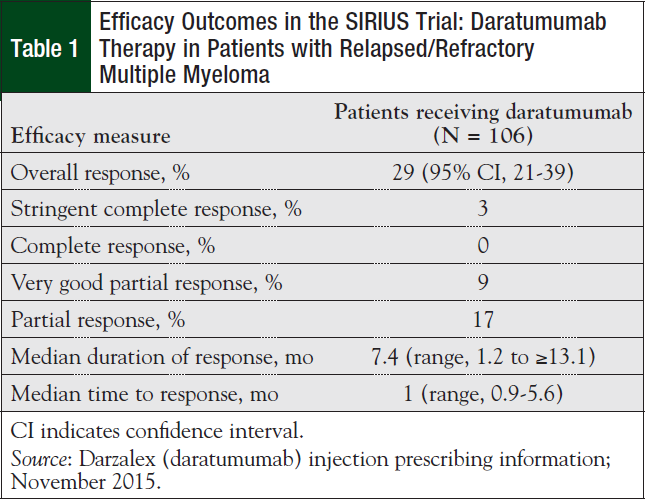
SIRIUS enrolled 106 patients with relapsed and/or refractory multiple myeloma. Daratumumab (16 mg/kg) was administered with preinfusion and postinfusion medications until unacceptable toxicity or until disease progression. The primary end point was the overall response rate as assessed by an Independent Review Committee using the International Myeloma Working Group criteria.13,14
The majority of patients enrolled in SIRIUS were female (51%) and white (79%). The patients’ median age was 64 years (range, 31-84 years). Patients had received a median of 5 previous therapies: 80% of patients had undergone autologous stem-cell transplantation; other previous therapies included bortezomib (99%), lenalidomide (99%), pomalidomide (63%), and carfilzomib (50%).13
At study enrollment, 97% of patients had disease refractory to their most recent line of treatment, 95% of patients had disease that was double-refractory to a proteasome inhibitor and an IMiD, and 77% of patients had disease refractory to alkylating agents.13
The overall response rate was 29%, which included 3% stringent complete responses, 9% very good partial responses, and 17% partial responses (Table 1).13,14 The median time to disease progression was 3.7 months, and the median overall survival has not been reached.14
The GEN501 Clinical Trial
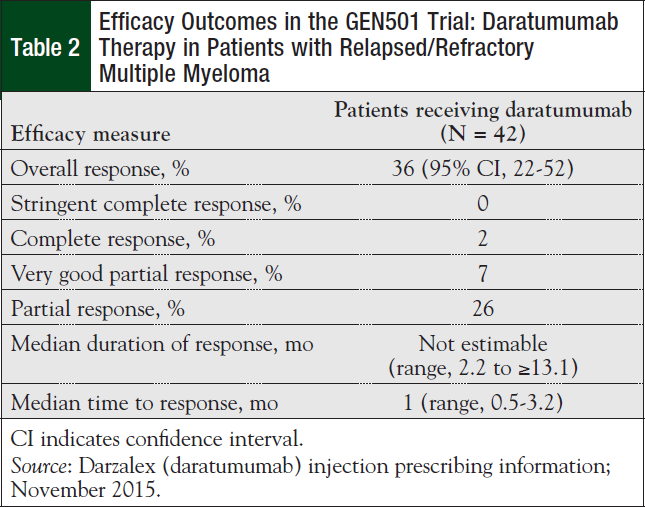
A total of 42 patients with relapsed and/or refractory multiple myeloma received daratumumab (16 mg/kg) in the GEN501 study.13,15 The primary end point was the overall response rate as assessed by an Independent Review Committee.13,15
The majority of patients in the GEN501 clinical trial were male (64%) and white (76%).13 The patients’ median age was 64 years (range, 44-76 years). Patients had received a median of 4 previous lines of therapy; 76% of patients had undergone autologous stem-cell transplantation. At study enrollment, 76% of patients had disease refractory to their most recent line of treatment for multiple myeloma, and 64% of patients had disease that was double-refractory to a proteasome inhibitor and an IMiD agent.13
The overall response rate was 36%, which included 1 complete response, 3 very good partial responses, and 11 partial responses (Table 2).13 The median duration of response has not been reached (range, 2.2 to ≥13.1 months).13,15 The median progression-free survival was 5.6 months.15
Adverse Events
The safety data for daratumumab are based on 156 adult patients with relapsed and/or refractory multiple myeloma who received 16 mg/kg of daratumumab in 3 open-label clinical trials. The median duration of exposure to daratumumab was 3.3 months, with a maximum of 20.4 months.13
Serious adverse reactions were reported in 33% of patients, including pneumonia (6%), general physical health deterioration (3%), and pyrexia (3%).13
Overall, 15% of patients taking daratumumab had treatment delay because of adverse reactions, most often because of infections. In addition, 4% of patients discontinued daratumumab because of adverse reactions.13
The most common (≥20%) adverse reactions (all grades) reported by the 156 patients who received daratumumab were infusion reactions (48%), fatigue (39%), nausea (27%), back pain (23%), pyrexia (21%), cough (21%), and upper respiratory tract infection (20%). None of these nonhematologic adverse reactions was life-threatening (grade 4).13
Grade 3 or 4 laboratory abnormalities reported at a rate of ≥10% with daratumumab included lymphopenia (40%), neutropenia (20%), anemia (19%), and thrombocytopenia (18%).13 Daratumumab has no contraindications, and no formal drug interaction studies have been conducted with daratumumab.13
Warnings and Precautions
Infusion reactions. Daratumumab can cause severe infusion reactions. Overall, 46% of patients receiving their first infusion of daratumumab experienced infusion reactions. None of the reactions in the second or subsequent infusions was grade ≥3. To reduce the risk for delayed infusion reactions, oral corticosteroids should be given on the first 2 days after each infusion. Patients with a history of obstructive pulmonary disorders may need additional postinfusion medications, such as short- and long-acting bronchodilators and inhaled corticosteroids.13
Interference with serologic testing. Daratumumab binds to CD38 on red blood cells, resulting in a positive indirect antiglobulin (Coombs) test result. This result can persist for up to 6 months after the last infusion. Blood transfusion centers should be notified of daratumumab’s interference with serologic testing, and blood banks should be informed that a patient has received daratumumab. Patients’ blood samples should be typed and screened before starting therapy with daratumumab.13
Interference with complete response determination. Daratumumab, a humanized IgG1 kappa monoclonal antibody, can be detected on the serum protein electrophoresis and immunofixation assays used to monitor endogenous M-protein levels. Determination of complete response and of disease progression can be affected in patients with IgG kappa myeloma protein.13
Specific Populations
Pregnancy. Based on its mechanism of action, daratumumab can cause fetal myeloid or lymphoid-cell depletion, and can affect bone density. The administration of live vaccines to neonates and infants who were exposed to daratumumab in utero should be deferred until a hematology evaluation is completed.13
Lactation. There is no information about daratumumab’s potential impact on human milk or on the breastfed infant. The benefits of breast-feeding should be considered relative to the mother’s need for daratumumab.13
Reproductive potential. Women of reproductive potential should use effective contraception during daratumumab treatment and for 3 months after treatment.13
Pediatric use. The safety and effectiveness of daratumumab in pediatric patients have not been established.13
Geriatric use. Overall, 45% of patients who received daratumumab were aged ≥65 years, and 10% of patients were aged ≥75 years. No differences in the safety or effectiveness of daratumumab were noted between older and younger patients.13
Renal impairment. No dose adjustment is necessary for patients with renal impairment.13
Hepatic impairment. No dose adjustment is necessary for patients with mild hepatic impairment. Daratumumab has not been studied in patients with moderate or severe hepatic impairment.13
Conclusion
Daratumumab is the first FDA-approved monoclonal antibody that targets CD38 that has demonstrated single-agent efficacy in patients with multiple myeloma who have received several previous treatments, including those whose disease is double-refractory to a proteasome inhibitor and an IMiD agent. To date, 2 clinical trials have demonstrated that this infused agent results in deep and durable responses.
Several clinical trials are under way to further establish the role of daratumumab in the treatment of patients with multiple myeloma, including phase 3 studies comparing daratumumab plus lenalidomide and dexamethasone versus the standard doublet therapy with lenalidomide and dexamethasone.17 The MAIA study is comparing these 2 regimens in patients with previously untreated multiple myeloma who are ineligible for high-dose therapy and autologous stem-cell transplantation, and the POLLUX clinical trial is comparing these regimens in patients with relapsed and/or refractory multiple myeloma.17,18
References
- National Cancer Institute. A snapshot of myeloma. November 5, 2014. www.cancer.gov/researchandfunding/snapshots/myeloma. Accessed December 15, 2015.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): multiple myeloma. Version 3.2016. January 15, 2016. www.nccn.org/professionals/physician_gls/pdf/myeloma.pdf. Accessed December 15, 2015.
- American Cancer Society. Multiple myeloma: what are the key statistics about multiple myeloma? Revised January 19, 2016. www.cancer.org/cancer/multiplemyeloma/detailedguide/multiple-myeloma-key-statistics. Accessed December 8, 2015.
- Smith L, McCourt O, Henrich M, et al. Multiple myeloma and physical activity: a scoping review. BMJ Open. 2015;5:e009576. Erratum in: BMJ Open. 2016;6:e009576corr1.
- Mayo Clinic staff. Diseases and conditions: multiple myeloma: treatments and drugs. December 4, 2015. www.mayoclinic.org/diseases-conditions/multiple-myeloma/basics/treatment/con-20026607. Accessed December 15, 2015.
- Kumar SK, Rajkumar SV, Dispenzieri A, et al. Improved survival in multiple myeloma and the impact of novel therapies. Blood. 2008;111:2516-2520.
- Andrews SW, Kabrah S, May JE, et al. Multiple myeloma: the bone marrow microenvironment and its relation to treatment. Br J Biomed Sci. 2013;70:110-120.
- Teitelbaum A, Ba-Mancini A, Huang H, Henk HJ. Health care costs and resource utilization, including patient burden, associated with novel-agent-based treatment versus other therapies for multiple myeloma: findings using real-world claims data. Oncologist. 2013;18:37-45.
- Garrison LP Jr, Wang S-T, Huang H, et al. The cost-effectiveness of initial treatment of multiple myeloma in the U.S. with bortezomib plus melphalan and prednisone versus thalidomide plus melphalan and prednisone or lenalidomide plus melphalan and prednisone with continuous lenalidomide maintenance treatment. Oncologist. 2013;18:27-36.
- Munshi NC, Anderson KC. New strategies in the treatment of multiple myeloma. Clin Cancer Res. 2013;19:3337-3344.
- Lee HC, Shah JJ, Orlowski RZ. Novel approaches to treatment of double-refractory multiple myeloma. Am Soc Clin Oncol Educ Book. 2013:e302-e306.
- US Food and Drug Administration. FDA approves Darzalex for patients with previously treated multiple myeloma. Press release. November 16, 2015. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm472875.htm. Accessed December 19, 2015.
- Darzalex (daratumumab) injection [prescribing information]. Horsham, PA: Janssen Biotech, Inc; November 2015.
- Lonial S, Weiss BM, Usmani SZ, et al. Phase II study of daratumumab (DARA) monotherapy in patients with ≥3 lines of prior therapy or double refractory multiple myeloma (MM): 54767414MMY2002 (Sirius). J Clin Oncol. 2015;33(18 suppl). Abstract LBA8512.
- Lokhorst HM, Plesner T, Laubach JP, et al. Targeting CD38 with daratumumab monotherapy in multiple myeloma. N Engl J Med. 2015;373:1207-1219.
- Smart Patients. Daratumumab (HuMax-CD38) Safety Study in Multiple Myeloma. www.smartpatients.com/trials/NCT00574288. Accessed December 21, 2015.
- ClinicalTrials.gov. Daratumumab. Search results. www.clinicaltrials.gov/ct2/results?term=daratumumab&Search=Search. Accessed December 21, 2015.
- Shaffer AT. Daratumumab combo sparks 81% response rate in myeloma. Onc Live. December 6, 2015. www.onclive.com/conference-coverage/ash-2015/daratumumab-combo-sparks-81-response-rate-in-myeloma. Accessed December 21, 2015.