Dr Brahim is Clinical Pharmacist, Dr Kernan is Assistant Pharmacy Director and Pharmacy Residency Director, Mr Ibrahim is Pharmaceutical Care Manager, Dr Nguyen is an associate staff member in oncology, and Dr Ohana is Pharmacist; all at Cleveland Clinic Florida, Weston.
Background: Mucositis is a significant adverse effect of chemotherapy that often leads to treatment delays or to dose reductions. Palifermin is a human keratinocyte growth factor that is indicated to decrease the incidence and the duration of severe oral mucositis in patients with hematologic malignancies who are receiving myelotoxic therapy requiring hematopoietic stem-cell support. Limited data are available concerning the efficacy and the safety of palifermin in the setting of solid tumors.
Objectives: To describe the use of palifermin outside of its US Food and Drug Administration– approved indication in a 70-year-old patient with stage IIIc squamous-cell anal carcinoma for the secondary prevention of oral mucositis when using fluorouracil plus mitomycin concurrent with radiation therapy.
Discussion: This patient was treated according to the Nigro protocol, and he experienced severe mucositis associated with his first 4 days of treatment (World Health Organization grade 3) with significant pain for more than 2 weeks. On day 32, a single dose of palifermin 180 mcg was administered as an intravenous bolus. The patient was able to receive full-dose chemotherapy and radiation and did not experience adverse effects related to taking palifermin. Mucositis was minimal, with no pain reported by the patient and only 2 small superficial ulcers noted on physical examination.
Conclusion: To our knowledge, there are no other case reports of the use of palifermin to prevent oral mucositis in a patient receiving high-dose fluorouracil plus mitomycin concurrent with radiation therapy. Although our patient experienced great benefit from treatment with no adverse effects, the use of palifermin in nonhematologic malignancies remains controversial because of the potential concern of tumor growth stimulation and of interference with clinical outcomes.
Mucositis is the inflammation of oral mucosa resulting from chemotherapeutic agents or ionizing radiation and is a significant adverse effect of cancer chemotherapy, as reported by patients.1-4 It typically manifests as erythema, which may progress to erosion and to severe ulcerations involving the oral cavity, oropharynx, and hypopharynx. The frequency of oral mucositis is estimated to be between 5% and 40% in patients receiving myelosuppressive chemotherapy for solid malignancies.1-4 It can lead to significant pain, requirement of total parenteral nutrition, systemic infections, increased number of hospitalizations, and increased length of stay.1-4
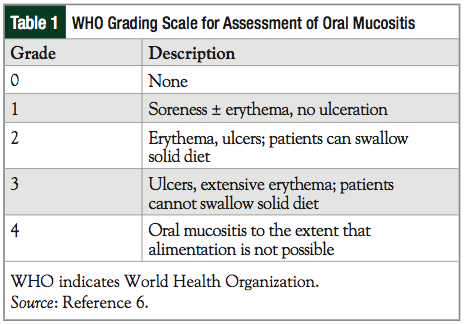
Mucositis is estimated to result in a dose reduction in approximately 23% to 28% of chemotherapy cycles.5 The risk for the development of oral mucositis may vary according to patient age, chemotherapy regimen, comorbidities, type of malignancy, and baseline oral condition. A variety of assessment scales have been developed. These scales consider mucosal changes, symptoms, and functional assessments. The World Health Organization (WHO) scale is one of the most widely used scales, and it grades mucositis from grades 1 to 4, with 4 being the most severe (Table 1).6
For patients who are at risk of developing oral mucositis, prevention and treatment options are limited. Effective oral hygiene (using soft toothbrushes, flossing, and using bland rinses, such as 0.9% saline, sodium bicarbonate, and water) and topical therapies, including topical anesthetics and mucosal-coating agents, are recommended by the Multinational Association of Supportive Care in Cancer and in the European Society for Medical Oncology clinical practice guidelines.1,2 Preventive oral cryotherapy is the application of ice chips to the oral cavity before and up to 30 minutes during the administration of antineoplastic agents.1,2 Cryotherapy may be useful in preventing the oral mucositis that is associated with chemotherapeutic agents administered as an intravenous (IV) bolus, such as 5-fluorouracil (5-FU).1,2,7 However, cryotherapy is not practical for continuous infusion chemotherapy.7
Palifermin is a human keratinocyte growth factor (KGF) produced by recombinant DNA technology in Escherichia coli.8-11 Endogenous KGF is a protein produced by mesenchymal cells in response to epithelial tissue injury. KGF binds to the KGF receptors and may result in the proliferation, differentiation, and migration of epithelial cells. KGF receptors have been detected in multiple tissues (eg, on the tongue, buccal mucosa, esophagus, stomach, and intestine).8-11
Palifermin is indicated to decrease the incidence and the duration of severe oral mucositis in patients with hematologic malignancies who are receiving myelotoxic therapy that requires hematopoietic stem-cell support.7 Palifermin’s mechanism of action is multifactorial. Palifermin increases the thickness of mucosal epithelium through its mitogenic effect, upregulates gene encoding for scavenging enzymes, and stimulates interleukin-13, which reduces tumor necrosis factor.1 In addition, palifermin exerts antiapoptotic effects and reduces angiogenesis.1,2
The recommended dose of palifermin is 60 mcg/kg administered as an IV bolus daily for 3 days before conditioning treatment and for 3 days after myelotoxic therapy, thereby totaling 6 doses.2,8 The efficacy of palifermin has not been established in patients with non-
hematologic malignancies.8
The following case report describes the off-label use of palifermin to prevent oral mucositis in a patient receiving fluorouracil, mitomycin, and radiation for anal cancer.
Case Report
A 70-year-old man was diagnosed with anal cancer after a biopsy revealed invasive, moderately differentiated stage IIIc squamous-cell carcinoma. A positron emission tomography scan showed positive anal lesion and bilateral inguinal lymph nodes. The patient’s medical history was significant for obstructed sleep apnea, osteoarthritis, and hyperlipidemia. His social history included smoking of 60 pack-years and consumption of approximately 15 oz to 18 oz of alcohol weekly (10-12 mixed drinks weekly). His home medications included fluticasone 50-mcg nasal spray at bedtime, atorvastatin 10 mg daily at bedtime, diazepam 10 mg daily at bedtime, hydrochlorothiazide 12.5 mg daily, transdermal testosterone daily, vitamin E 100 U daily, and oxycodone plus acetaminophen 10/650 mg every 6 hours as needed for pain.
Three weeks after his diagnosis, the patient was initiated on concurrent chemoradiation according to the Nigro regimen. The regimen consisted of 5-FU 1000 mg/m2 daily (actual dose, 2100 mg over 24 hours) continuous IV infusion on days 1 to 4 and on days 29 to 32, and mitomycin 10 mg/m2 (actual dose, 21 mg) as an IV bolus on days 1 and 29, concurrent with radiation therapy of 1.8 Gy daily, 5 days weekly for 5 weeks (total, 45 Gy). Before the first treatment, the review of systems and the patient’s physical examination were normal. His only complaint was some perianal discomfort and infrequent bleeding. The patient was otherwise healthy with an Eastern Cooperative Oncology Group Performance Status grade of 0.12
On day 6, the patient was seen by the oncologist and was found to have developed WHO grade 3 mucositis; oral mucosa was noted to be red with ulcer lesions and fissures at the corners of the lips. The patient described the pain as a 10 (on a scale of 0-10), with a burning, constant pain and the inability to swallow solid food, which started on day 3. The patient was still able to swallow liquids and medications. Pain management was initiated with oxycodone plus acetaminophen 10/325 mg every 4 hours as needed for pain, and fentanyl 25-mcg transdermal patch applied every 72 hours. Oral rinses every 4 hours with 5 mL to 10 mL of magic mouthwash (antacid, 30 mL; viscous lidocaine 2%, 50 mL; nystatin oral suspension 100,000 U/mL, 30 mL) and saline solution were started as well.
On day 10, the patient developed grade 3 neutropenia, and his laboratory values showed a white blood cell count of 1.1 K/µL and an absolute neutrophil count of 0.5 K/µL. The patient reported a pain level of 8 (scale, 0-10) despite taking pain medications as prescribed. The oral cavity was described as having moist oral mucosa, erythema of the tongue with small visible ulcers, and generalized redness. The decision was made to hold radiation from day 10 and to restart it on day 15 because of mucositis and neutropenia, and to start the patient on filgrastim 480 mcg daily subcutaneously for 3 days. The patient was instructed to continue using oral rinses (ie, magic mouthwash, baking soda, and salt solution).
On day 14, a physical examination revealed partial recovery of mucous membranes, although the patient still verbalized a pain level in the mouth of 8 and trouble swallowing. On day 17, a physical examination revealed moist oral mucosa without lesions, and the pain was rated as 4 on a scale of 0 to 10. On day 23, a physical examination revealed moist oral mucosa with erythema with no ulcer, and the patient rated his pain level as 0.
When the patient experienced 13 days of mucositis after chemotherapy treatment days 1 to 4, he refused further treatment out of fear of developing mucositis, despite several patient–provider discussions. The patient’s refusal led to a treatment delay. To address his concerns and to minimize subsequent toxicities, a number of options were evaluated, including a 25% dose reduction of the overall regimen and/or the omission of mitomycin from the regimen. However, these alternatives could possibly compromise the treatment’s effectiveness.
The option of a one-time dose of palifermin was presented to the physician and to the patient, although evidence of use in this setting was lacking. The decision was made to use palifermin off label as a single dose 3 days before the initiation of chemotherapy on day 35. The patient consented with this plan.
At 72 hours before receiving chemotherapy, the patient was administered palifermin 180 mcg/kg as an IV bolus in a single dose in the outpatient clinic, which the patient tolerated well. He was monitored in the infusion center for 2 hours postadministration and then discharged home. He also received filgrastim 480 mcg daily subcutaneously for 2 days on days 33 and 34 as prophylaxis for neutropenia. The patient was given education about the importance of good oral hygiene and about smoking cessation, but he never stopped smoking.
Chemotherapy was started on day 35. The patient received a full dose of fluorouracil 1000 mg/m2 daily (actual dose, 2100 mg over 24 hours) in a continuous IV infusion on days 35 to 39 and mitomycin 10 mg/m2 (actual dose, 21 mg) as an IV bolus on day 35. During a follow-up visit on day 39, the patient reported to be pain free, and a physical examination revealed moist oral mucosa without lesions.
In an interview with the patient, he stated that he did not experience any mucositis-related pain. On day 46, the patient came to the emergency department with a chief complaint of fever and chills and was admitted (temperature, 100°F; white blood cell count, 0.4 K/µL; absolute neutrophil count, 0.2 K/µL), where he received IV vancomycin and piperacillin plus tazobactam. On physical examination during this admission, the patient was noted as having pink mucous membranes, except for 2 small superficial ulcers.
The patient was discharged on day 49. Blood cultures that were taken on day 46 showed no growth at 5 days. During a follow-up visit on day 50, the physical examination revealed moist oral mucosa with 2 superficial oral ulcers and no mouth pain. The patient denied dysphagia and odynophagia. On day 66, he had no change of appetite, energy, or weight, and his oral mucosa was noted to be moist without lesions.
During a follow-up interview with the patient approximately 1 month after completion of the chemoradiation therapy, he stated that he experienced no mucositis-related pain. One year after completing treatment, he has no evidence of new soft tissue masses seen on computed tomography scan at 3 months, 6 months, 12 months, and 18 months posttreatment. The patient follows up regularly with the oncologist and with the colorectal surgeon.
Discussion
Patients may experience increased toxicities associated with their cancer treatments now that more intensive cancer therapies, including radiation, cytotoxic chemotherapy, and biologic-targeted therapies, are being used. One of the most significant of these toxicities is mucositis. Oral mucositis oftentimes is a dose-limiting toxicity.5
The development and evaluation of supportive agents that improve patients’ quality of life, as well as clinical outcomes, are critical. By stimulating epithelial-cell proliferative activity, palifermin has a unique mechanism of action that is useful for the prevention of mucositis.
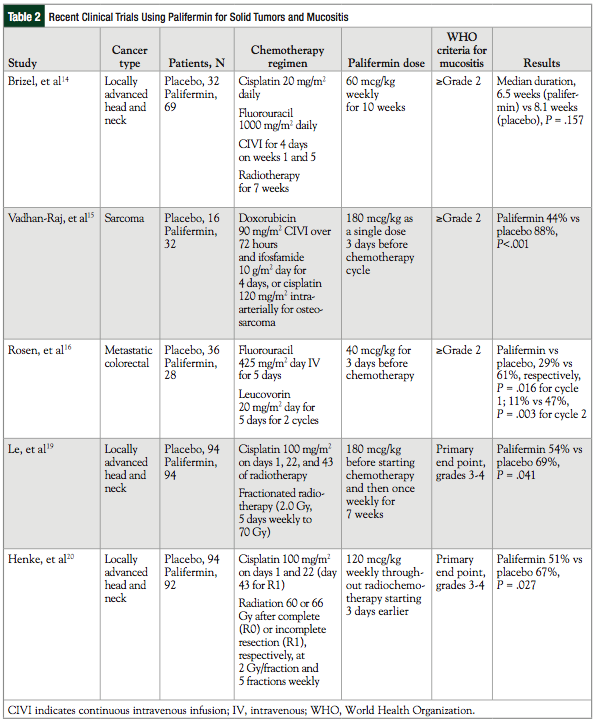
The use of palifermin in hematologic malignancies and stem-cell transplants has been established, but its efficacy in nonhematologic malignancies has yet to be conclusively determined.13 Several clinical trials have evaluated the use of palifermin in the prevention of mucositis in patients with solid tumors.14-19 A PubMed search for clinical trials that was limited to the past 15 years using the key words “palifermin,” “solid tumors,” and “mucositis” yielded several articles, as listed below and in Table 2.
A phase 1/2 randomized, double-blind, placebo-controlled study was conducted of patients with metastatic colorectal cancer who were receiving fluorouracil-based chemotherapy.16 Patients received leucovorin 20 mg/m2 administered by IV injection, immediately followed by an IV bolus of fluorouracil 425 mg/m2 once daily for 5 consecutive days. Patients received 2 chemotherapy cycles. The patients in the treatment arm received IV palifermin 40 mcg/kg daily for 3 consecutive days before chemotherapy.
The efficacy outcomes included incidence, duration, and severity of mucositis (WHO grades 2-4). Safety evaluations included adverse events, clinical laboratory values, and the development of antipalifermin antibodies. The incidence of WHO grade 2 or higher mucositis was significantly lower in the palifermin group versus in the group receiving placebo (29% vs 61%; P = .016). The overall incidence of adverse events was comparable between the study groups. One patient in the study developed antipalifermin antibodies; titers were below the quantitation limit. Of note, fewer patients in the palifermin group required a chemotherapy dose reduction during cycle 2 than patients in the placebo group.
Vadhan-Raj and colleagues conducted a randomized, double-blind, placebo-controlled trial to evaluate the efficacy of palifermin when it is given as a single dose before each cycle of chemotherapy in 48 patients with sarcoma who had already experienced severe mucositis.15 Patients were given palifermin 180 mcg/kg or placebo intravenously as a single dose 3 days before chemotherapy with doxorubicin and ifosfamide in each cycle.
The primary end point was the incidence of moderate-to-severe mucositis (≥grade 2). Patients in the palifermin group experienced a lower incidence of grade 2 or higher mucositis versus the placebo group (44% vs 88%, respectively; P <.001). Common adverse events included patient-reported sensation of increased thickness of oral mucosa, altered taste, and a film coating in the mouth.
A phase 2 trial evaluated the efficacy of palifermin in patients receiving concurrent chemoradiotherapy for advanced head and neck squamous-cell carcinoma.14 Patients in the treatment arm were given 60 mcg/kg of palifermin once weekly for 10 doses.
The primary outcome of median duration of grade 2 or greater mucositis was shorter for palifermin than for placebo (6.5 and 8.1 weeks, respectively), but the difference was not significant (P = .157). The proportion of patients who still had grade 2 mucositis at week 12 was 47% in the palifermin group and 42% in the placebo group. The authors noted that the palifermin dose may have been too low to show a significant difference, because the study was powered to detect a mean difference of 30%, based on results from a previous trial.14
Le and colleagues conducted a multicenter, double-blind study of 188 patients receiving postoperative concurrent chemoradiotherapy (2.0 Gy daily, 5 days weekly, to 70 Gy) with cisplatin (100 mg/m2 on days 1, 22, and 43) for locally advanced head and neck squamous-cell carcinoma.19 The patients in the study arm received palifermin 120 mcg/kg 3 days before treatment and then weekly for 7 weeks. The primary end point was the incidence of severe mucositis (WHO grades 3-4), in which significance was reached (54% vs 69%, respectively; P = .041). Overall survival and progression-free survival were similar between the 2 arms after a median follow-up of almost 26 months.
Henke and colleagues studied the efficacy of palifermin in patients who were undergoing postoperative radiochemotherapy for head and neck cancer.20 This multicenter, double-blind, randomized trial enrolled 92 patients in the palifermin arm and 94 patients in the placebo arm. Patients received 60 Gy or 66 Gy of radiochemotherapy after complete (R0) or incomplete (R1) resection, respectively, at 2 Gy per fraction and 5 fractions weekly. Cisplatin 100 mg/m2 was administered on days 1 and 22 (and on day 43 with R1 resection). Patients were randomly assigned to receive weekly palifermin 120 mcg/kg or placebo from 3 days before radiochemotherapy and continuing throughout radiochemotherapy.
The primary end point was the incidence of severe oral mucositis (WHO grades 3-4). Patients in the palifermin group experienced severe oral mucositis at a significantly lower rate (51% vs 67%, respectively; P = .027) than in the placebo group. Adverse effects were similar between the 2 groups. Survival times for the palifermin and the placebo arms were nearly identical after a median follow-up of almost 33 months. The investigators cautioned against generalization of these results because of their small sample size.
The use of palifermin in the setting of solid tumors raises questions that are not applicable to the treatment of patients with hematologic malignancies, because epithelial cells express KGF receptors, whereas blood cells do not.17 A concern of using palifermin for multiple doses up to the day before chemotherapy for repeated cycles is that because mucosal tissue is rapidly proliferating, it may be more sensitive to chemotherapy-induced injury. In addition, if tumors were to express the KGF receptors, the administration of palifermin could theoretically lead to the stimulation of tumor growth and therefore interfere with disease outcomes, although in vitro and in vivo studies do not indicate a definitive role for KGF in tumor genesis.17 However, if the medication is given as a single dose, this issue may be avoided. Clinical studies that were conducted in patients with hematologic and solid tumor cancer did not show adverse clinical outcomes.14-16,18-20
Furthermore, in a phase 2 study of patients with head and neck squamous-cell carcinoma, mucosal cells in patients who were given a single dose of palifermin were shown to express cyclin E, a putative G1 marker, thereby suggesting that most of the mucosal cells were not actively dividing.15 In light of the experiences with erythropoietin-stimulating agents and their effect on tumor growth, it is important to assess the long-term safety of this KGF.
The patient described in this case report had several risk factors for the development of oral mucositis. Fluorouracil is known to be one of the agents with the highest risk of developing mucositis, and the addition of radiation to chemotherapy further increases this risk.1,2 Delaying radiation treatment, as was done during the first cycle, has been documented to lead to poorer outcomes.21 Additional patient-specific risk factors included his continued alcohol consumption and his tobacco use.
The patient received a dose of 180 mcg/kg of palifermin, corresponding to the dose that was used in the above-mentioned clinical trial by Vadhan-Raj and colleagues, which was available at the time.15 The study by Vadhan-Raj and colleagues also established the efficacy of palifermin as prophylaxis in patients who already experienced severe mucositis, as our patient did. Subsequent trials that were conducted in patients with head and neck cancer have been published with alternative dosing regimens with varying results. However, no data were available about the use of palifermin in a regimen of fluorouracil 1000 mg/m2 plus mitomycin 100 mg/m2 concurrent with radiation.
Our patient tolerated palifermin very well, with no complaints of adverse effects, which is consistent with experiences in the literature. The side effects tend to be mild for most patients, including altered taste and dry mouth.
To date, the patient described in this case report did not suffer any adverse clinical outcomes that could possibly be linked to his use of palifermin. However, we still have limited data on the use of palifermin in multiple doses for repeated cycles on clinical outcomes, such as survival rate and time to disease progression.
Our decision to use palifermin was made after other therapies (ie, oral rinses, cryotherapy) had failed to relieve the patient’s symptoms. Furthermore, our patient was refusing the continuation of chemoradiation, even though his disease was very curable. The positive experience from this case report cannot necessarily be extrapolated to patients with solid tumors, who are at a lower risk for developing mucositis.
Conclusion
Clinical trials of palifermin use in patients with solid tumors show promise, but there is little consistency across studies concerning dosing and primary end points. No clinical trials have evaluated the use of palifermin in high-dose fluorouracil therapy combined with radiation, such as the Nigro regimen. To our knowledge this is the first report of palifermin being used in a patient with anal cancer for the prevention of mucositis. Further research for the long-term safety and efficacy of palifermin in patients with nonhematologic malignancies is warranted. Palifermin may only be an option once other therapies are exhausted because of its possible effects on patient outcomes, especially in early-stage solid-tumor cancers. An extensive patient-specific risk-versus-benefit analysis needs to be conducted before using palifermin in this setting.
Author Disclosure Statement
Dr Brahim, Dr Kernan, Mr Ibrahim, Dr Nguyen, and Dr Ohana reported no conflicts of interest.
References
1. Keefe DM, Schubert MM, Elting LS, et al; Mucositis Study Section of the Multinational Association of Supportive Care in Cancer and the International Society for Oral Oncology. Updated clinical practice guidelines for the prevention and treatment of mucositis. Cancer. 2007;109:820-831.
2. Peterson DE, Bensadoun RJ, Roila F; ESMO Guidelines Working Group. Management of oral and gastrointestinal mucositis: ESMO clinical recommendations. Ann Oncol. 2009;20(suppl 4):174-177.
3. Treister NS, Woo S-B. Chemotherapy-induced oral mucositis. MedScape. Updated April 23, 2013. http://emedicine.medscape.com/article/1079570-over view. Accessed April 25, 2013.
4. Borbasi S, Cameron K, Quested B, et al. More than a sore mouth: patients’ experience of oral mucositis. Oncol Nurs Forum. 2002;29:1051-1057.
5. Elting LS, Cooksley C, Chambers M, et al. The burdens of cancer therapy: clinical and economic outcomes of chemotherapy-induced mucositis. Cancer. 2003;98:1531-1539.
6. World Health Organization. WHO Handbook for Reporting Results of Cancer Treatment. Geneva, Switzerland: World Health Organization. 1979. http://whqlib doc.who.int/offset/WHO_OFFSET_48.pdf. Accessed April 2, 2013.
7. Rubenstein EB, Peterson DE, Schubert M, et al; Mucositis Study Section of the Multinational Association for Supportive Care in Cancer, International Society for Oral Oncology. Clinical practice guidelines for the prevention and treatment of cancer therapy-induced oral and gastrointestinal mucositis. Cancer. 2004;100(9 suppl):2026-2046.
8. Kepivance (palifermin) [prescribing information]. Stockholm, Sweden: Swedish Orphan Biovitrum AB; November 2011.
9. Osslund TD, Syed R, Singer E, et al. Correlation between the 1.6 A crystal structure and mutational analysis of keratinocyte growth factor. Protein Sci. 1998;7:1681-1690.
10. Danilenko DM. Preclinical and early clinical development of keratinocyte growth factor, an epithelial-specific tissue growth factor. Toxicol Pathol. 1999;27:64-71.
11. Werner S. Keratinocyte growth factor: a unique player in epithelial repair processes. Cytokine Growth Factor Rev. 1998;9:153-165.
12. Oken MM, Creech RH, Tormey DC, et al. Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5:649-655.
13. Spielberger R, Emmanouilides C, Stiff P, et al. Use of recombinant human keratinocyte growth factor (palifermin) can reduce severe oral mucositis in patients with hematologic malignancies undergoing autologous peripheral blood progenitor cell transplantation after radiation-based conditioning. J Support Oncol. 2004;2(suppl 2):73-74.
14. Brizel DM, Murphy BA, Rosenthal DI, et al. Phase II study of palifermin and concurrent chemoradiation in head and neck squamous cell carcinoma. J Clin Oncol. 2008;26:2489-2496.
15. Vadhan-Raj S, Trent J, Patel S, et al. Single-dose palifermin prevents severe oral mucositis during multicycle chemotherapy in patients with cancer: a randomized trial. Ann Intern Med. 2010;153:358-367.
16. Rosen LS, Abdi E, Davis ID, et al. Palifermin reduces the incidence of oral mucositis in patients with metastatic colorectal cancer treated with fluorouracil-based chemotherapy. J Clin Oncol. 2006;24:5194-5200.
17. Finch PW, Rubin JS. Keratinocyte growth factor expression and activity in cancer: implications for use in patients with solid tumors. J Natl Cancer Inst. 2006;98:812-824.
18. Bossi P, Locati LD, Licitra L. Palifermin in prevention of head and neck cancer radiation-induced mucositis: not yet a definitive word on safety and efficacy profile. J Clin Oncol. 2012;30:564-565.
19. Le QT, Kim HE, Schneider CJ, et al. Palifermin reduces severe mucositis in definitive chemoradiotherapy of locally advanced head and neck cancer: a randomized, placebo-controlled study. J Clin Oncol. 2011;29:2808-2814.
20. Henke M, Alfonsi M, Foa P, et al. Palifermin decreases severe oral mucositis of patients undergoing postoperative radiochemotherapy for head and neck cancer: a randomized, placebo-controlled trial. J Clin Oncol. 2011;29:2815-2820.
21. Pepek JM, Willet CG, Czito BG. Radiation therapy advances for treatment of anal cancer. J Natl Compr Canc Netw. 2010;8:123-129.